Overview
There is mounting interest in the use of psychedelics as standalone therapies or combined with psychotherapy, holding the potential to transform the way we treat mental health conditions. According to the World Health Organization, 1 in every 8 people globally were living with a mental disorder in 2019, with depressive and anxiety disorders being the most prevalent. Studies have reported that up to 30% of adults with major depressive disorders are resistant to pharmacotherapy, which is defined as having no response to at least two different antidepressant treatments.
Additionally, some patients exhibit severe side effects, leading to a continued high unmet need for more effective treatments. As psychedelic assets continue to progress through the clinical development pathway, and as regulation, public acceptance and supporting infrastructure become increasingly favourable, the next 10 to 20 years are likely to see a transformation in the patient journey for many mental health conditions.
In this Executive Insights, L.E.K. Consulting examines the exciting possibilities for a revolutionised patient journey in mental health, overcoming many of the existing challenges in today’s care pathway.
Current challenges in the patient journey
A range of challenges across the patient journey currently plague patients who have mental health conditions. Societal stigma and misconceptions may hinder individuals from seeking treatment in the first place. Limited options for effective pharmacological treatments can impede recovery. Additionally, the availability and affordability of talking therapies can be limited; clinics and therapists face capacity constraints, resulting in extended waiting times for patients. Inadequate patient monitoring to ensure adherence to treatment plans is a further challenge impeding patient care today.
In the Global Burden Disease Study 2019, mental disorders were attributed to over 125 million disability-adjusted life years (5% of the global burden). Poor mental health cost the world economy over $2.5 trillion in terms of poor health and reduced productivity in 2010, with a projected rise to $6 trillion by 2030. Furthermore, comorbidities, such as arrhythmia, chronic kidney disease, anaemia, chronic heart failure, diabetes, hypertension and rheumatoid arthritis, were more commonly observed in depression patients than in the general population. Given the significant burden of mental disorders, it is imperative for society to take proactive steps in order to improve the patient journey and outcomes for individuals in the future.
Charting the path: The patient journey in 2040 and beyond, across five stages
With a significant portion of individuals not responding to pharmacotherapy or psychotherapies for a range of mental illnesses, there is a pressing need for alternative approaches to mental health treatment.
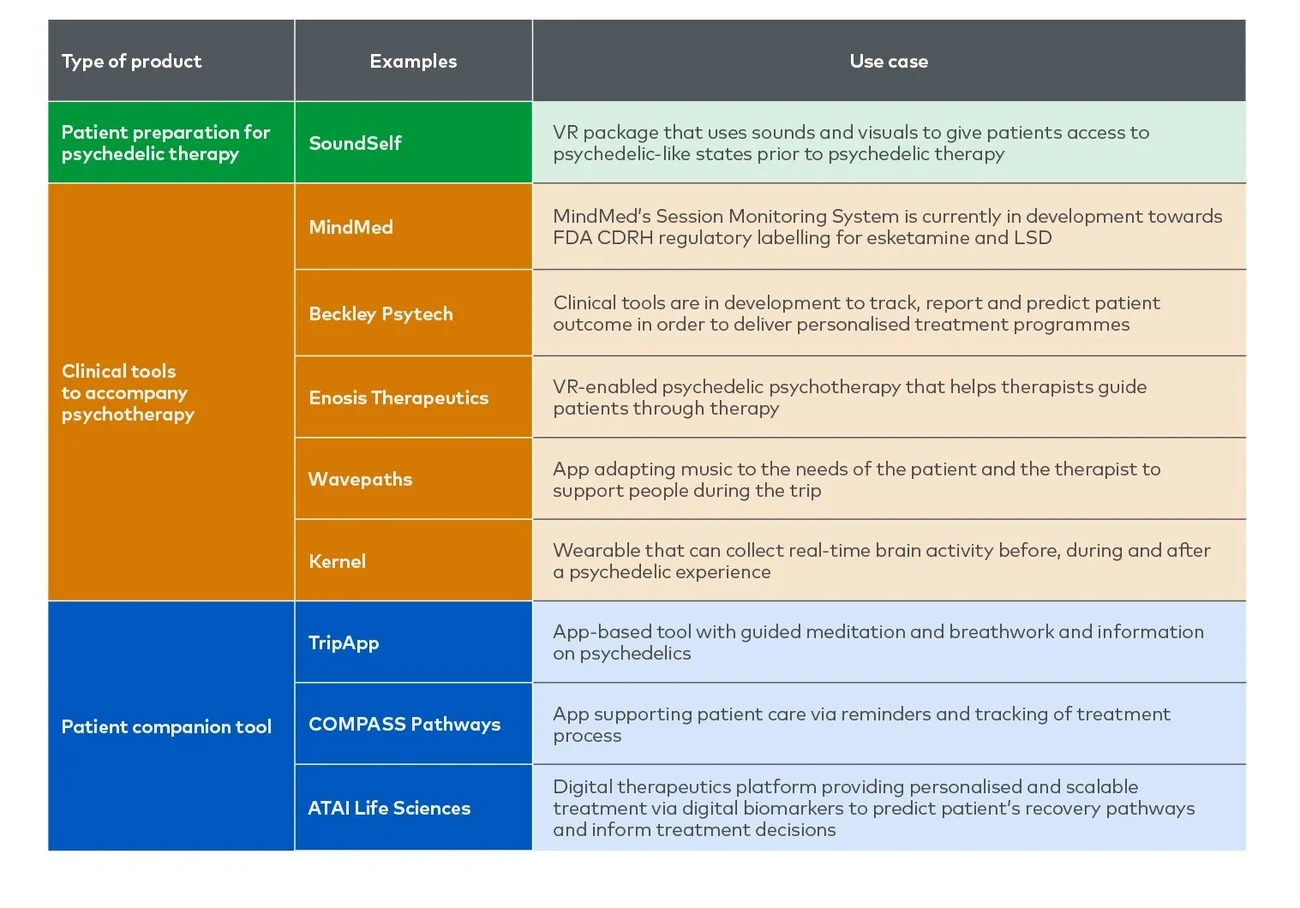
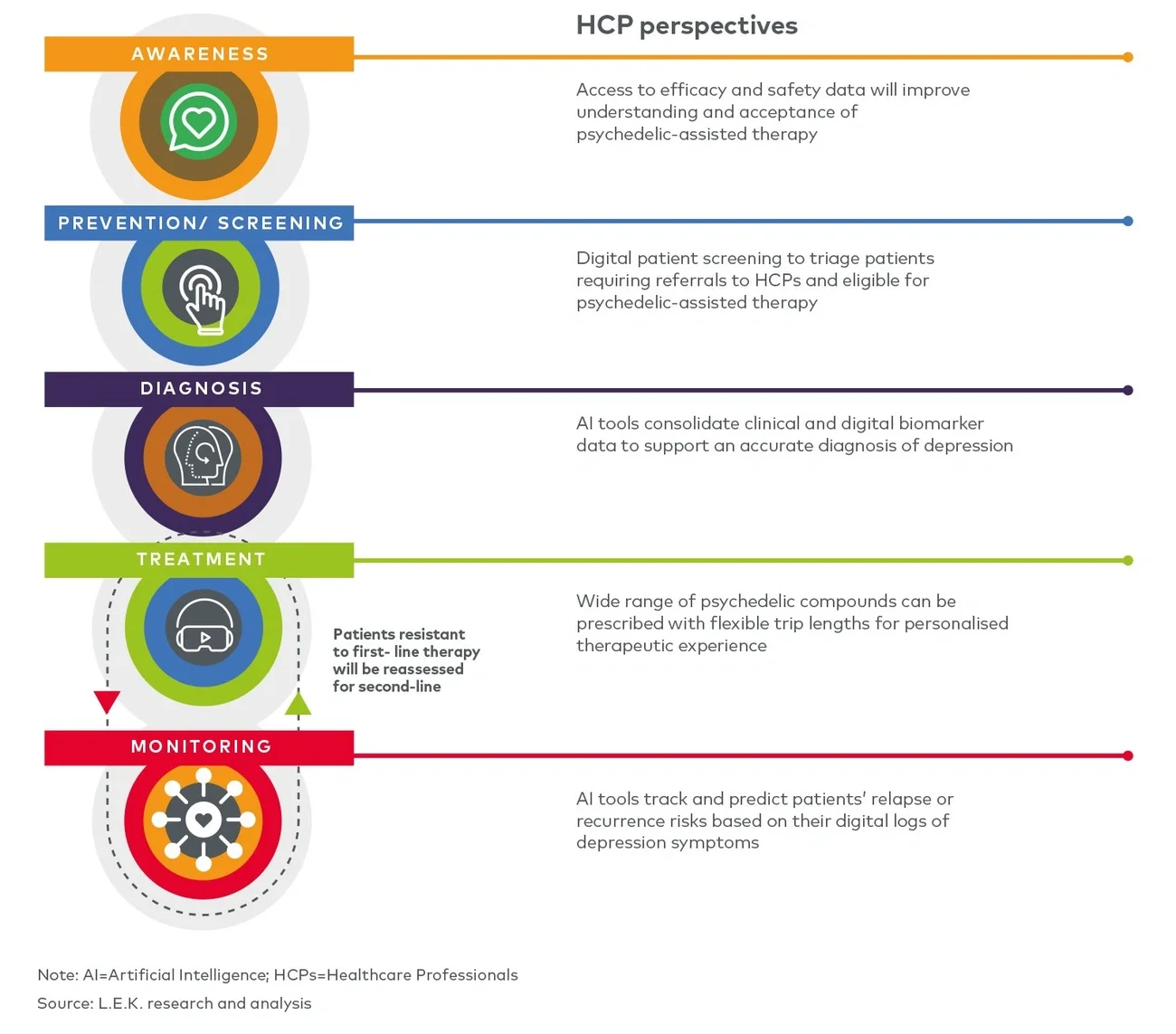
Psychedelic therapy has emerged as a promising avenue to treat illnesses — including depression, anxiety, post-traumatic stress disorder (PTSD) and addiction — providing the impetus for change with their recent proven benefits in clinical trials. As psychedelic therapies gain wider recognition as potential game changers in mental healthcare by 2040, it becomes essential to create a positive patient journey involving the safe use of psychedelics in a supportive environment. In this Executive Insights, we focus on the patient journey for depression (see Figure 1).