The US Food and Drug Administration for instance has streamlined its communications and turnaround times, as well as making greater use of umbrella trials and emergency use authorizations to dramatically accelerate development timelines for all virus countermeasures.
The FDA already plans to make aspects of its acceleration efforts around the pandemic permanent, and the potential for multiple disease areas is exciting. This was noted by one senior executive at a large pharmaceutical company, who commented: “The most impressive thing to me has been the regulatory streamlining and use of EUAs to really accelerate development – why can’t we do this in areas with high existing unmet need outside of a pandemic?”
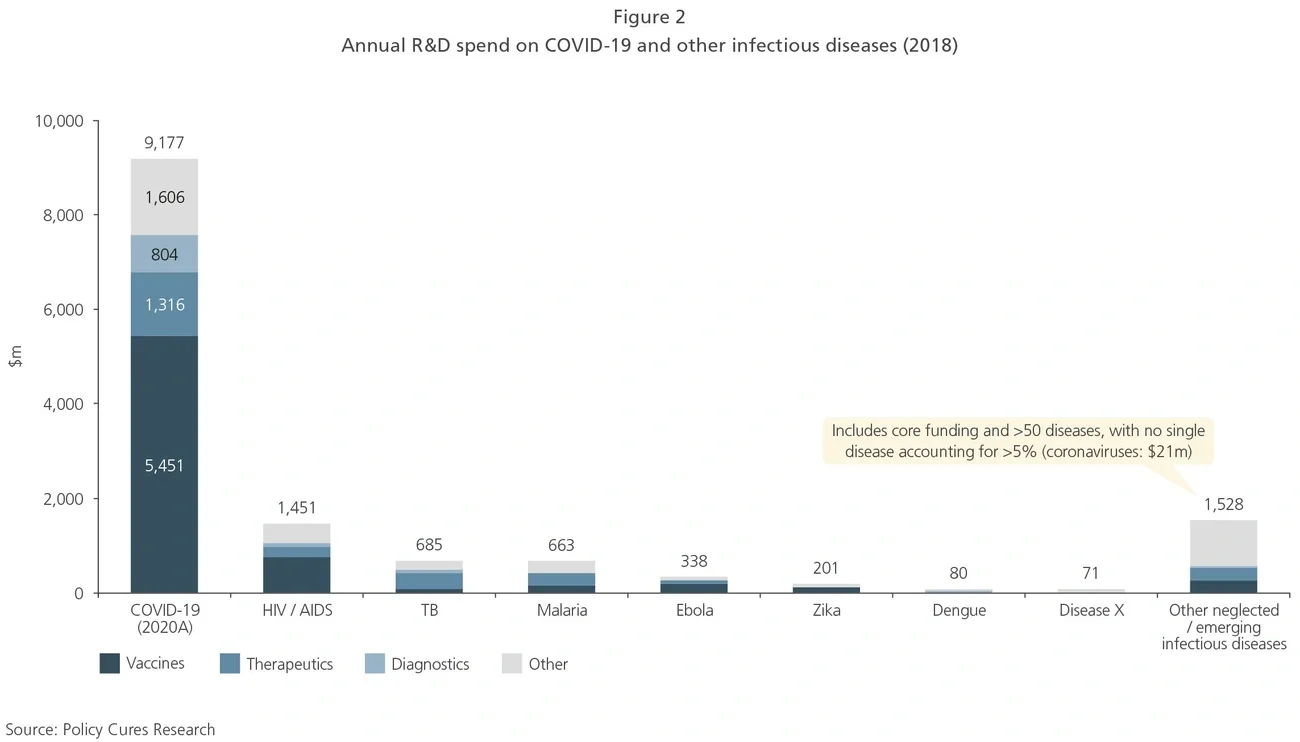
More broadly, the level of R&D investment in COVID-19 over the past year has dwarfed that seen in other infectious diseases, even those with extremely high burdens (see Exhibit 3). Witnessing the success of development programs with such significant financial backing raises the hope that neglected infectious diseases could also see greater and faster progress through larger investment.
Furthermore, Joe Simmonds-Issler, chief of staff of the Coalition for Epidemic Preparedness Innovations (CEPI), believes that technologies that have been validated in response to this pandemic, such as mRNA or adenovirus vaccines, may have direct applications for other diseases. He said: “The University of Oxford are working on other diseases for their adenovirus vaccine platform, and their processes will be more validated and streamlined through this experience.”
Lesson 6: Increase Data Transparency And Collaboration
This pandemic has also demonstrated the need for, and benefits from, data transparency and collaboration. Michele Robbins, a pharmaceutical executive with more than 20 years’ experience working in HIV, said: “We witnessed the importance of sharing scientific and clinical results quickly amongst different organizations and institutions. Sharing the data certainly contributed to finding solutions more quickly and more cost- effectively.”
Countries such as the US, the UK, France and Germany have sometimes suffered from having data that is fragmented and hard to access, while researchers stress the need for centralized and simplified sources to track, for example, epidemiology and patient outcomes.
Collaborative efforts to address this problem have, though, been evident, including those arising from pharmaceutical company alliances (e.g. between GlaxoSmithKline plc and Sanofi) and pharma-academia collaborations (e.g. between AstraZeneca PLC and Oxford University), as observed by Jacopo Andreose, SVP, Gilead, who said: “The infectious disease sector has always been relatively collaborative but this level is new advocates for collaboration within our industry are being really vocal.”
These partnerships have allowed companies to focus on their strengths, pool resources and drive innovation, with great potential for progress in other diseases.
COVID-19 has also brought about increased coordination and collaboration, as well as investment in product commercialization, specifically in manufacturing and distribution. Multiple organizations, most notably CEPI and the US government’s Operation Warp Speed, have spent billions of dollars funding the manufacture of vaccines and therapeutics “at risk,” to minimize waiting times, if they are found to be effective and safe.
The world is set to reap the benefits of this with billions of vaccine doses likely to be available throughout 2021. Paul Barnsley, of the think tank Policy Cures Research, states that the logic of manufacturing at risk to reduce timelines could be extended to other high-burden diseases: “We are manufacturing at risk to get the vaccine out there as quickly as possible and save as many lives as possible. This argument for saving lives by saving time applies equally to diseases like HIV and TB as well.”
Lesson 7: Improve Medical Access For Both Physical And Mental Health
A society’s ability to defeat infection is predicated on comprehensive access for its citizens to vaccines, testing and treatment. This is especially true with diseases where patients are infectious before symptoms arise, or where infection is a source of stigma. This is true for COVID-19 but also diseases such as HIV and hepatitis C. Beatriz García Fidalgo, of Abbott Laboratories Ltd comments: “In the absence of a vaccine, defeating these diseases is contingent upon identifying high-risk groups and then proactively screening them and offering treatment; by the time they show up at the doctor’s office it’s often too late.”
COVID-19 has also highlighted the mental health impacts of disease: mental health impairment from the pandemic is estimated to have cost the US$1.5trn so far, according to a recent report in JAMA, either from direct symptoms (“Long COVID”) or related to stay-at- home measures. Whilst the burden of COVID-19 is deeply regrettable, there are significant mental health implications of other infectious diseases too, and the focus on the psycho-social elements of these diseases particularly ones with chronic or extended duration such as HIV, hepatitis and TB – is likely to be welcome.
Patients
Lesson 8: Boost Public Health Measures
Non-pharmaceutical public health measures themselves can often be the most powerful tools against an infectious disease if they are embraced by individuals and groups. The need for, and importance of, public health awareness has never been clearer: a study published by the New York Times in November 2020 showed a striking association between the stringency of US states’ containment measures and their relative numbers of COVID-19-related hospitalizations.
Blythe Adamson, a leading infectious diseases epidemiologist and affiliate professor at the University of Washington, agrees. She said: “The social determinants of health are often overlooked but I think that the COVID experience has engendered greater empathy for their importance.”
Non-pharmaceutical interventions, such as “social distancing,” undertaken for COVID, also seem to be effective against a broader range of respiratory diseases, including TB and influenza. One senior executive at a large pharmaceutical company said: “If everyone were to follow the same measures for TB as for COVID, we would see astronomical decreases in patient numbers.” In the case of influenza, the southern hemisphere’s winter spike did not materialize in 2020, and it appears to be significantly curtailed in the beginnings of the northern hemisphere’s winter as well.
Lesson 9: Focus On Messaging And Maintenance Of Public Trust
The effectiveness of public health measures, as well as that of vaccines and therapeutics, is contingent on the public’s acceptance of them. The need for clear, consistent, and coordinated messaging has been demonstrated in the struggles of multiple countries, as well as the success of nations such as China, South Korea and New Zealand.
Changing behavior can be incredibly powerful but is also very difficult and requires a lot of focus from governments,” said an infectious diseases pharmacist in a UK hospital. This principle applies to all infectious diseases, from controlling STIs to maximizing vaccine uptake for influenza and previously common childhood infections. The same point can also be made for the importance of combating misinformation, which was already an issue for vaccines and other medicines but has been amplified during this pandemic.
Lesson 10: Invest In Digital Health Technology
Digital health technology has proved an important tool during the COVID-19 pandemic. Rapidly developed digital solutions in various fields including screening, clinical management, planning and tracking, medical supplies, contact tracing and quarantine/self-isolation have all played a role in containing or helping to manage the infection rate. There is emerging evidence for countries such as South Korea that indicate that flatter infection incidence curves are attributable, at least in part, to better adoption of digital technologies.
In particular, the innovation in digital solutions that aid patients’ fight against disease (with due consideration for data protection) has been notable. Contact tracing apps and the first rapid home tests have been successfully rolled out; these advancements may have lasting benefit in the fight against other diseases. One leading infectious diseases physician said “If we think about some infectious diseases like RSV, there are now rapid tests that can give you results within minutes which are as accurate as samples sent to the lab. For infectious diseases where contact tracing is required, digital health technology could be adopted to improve existing systems.”
Lasting Change
The health care, social and economic effects of COVID-19 will continue to be felt for years, if not decades to come. We have already witnessed a transition away from pre-COVID approaches and behaviors, such as large offices or a reliance on face-to-face health care. Similarly, pre-existing trends around remote working and telehealth have been accelerated. There is also the potential for new practices to emerge from this pandemic, such as R&D and regulatory reforms and new, improved public health strategies.
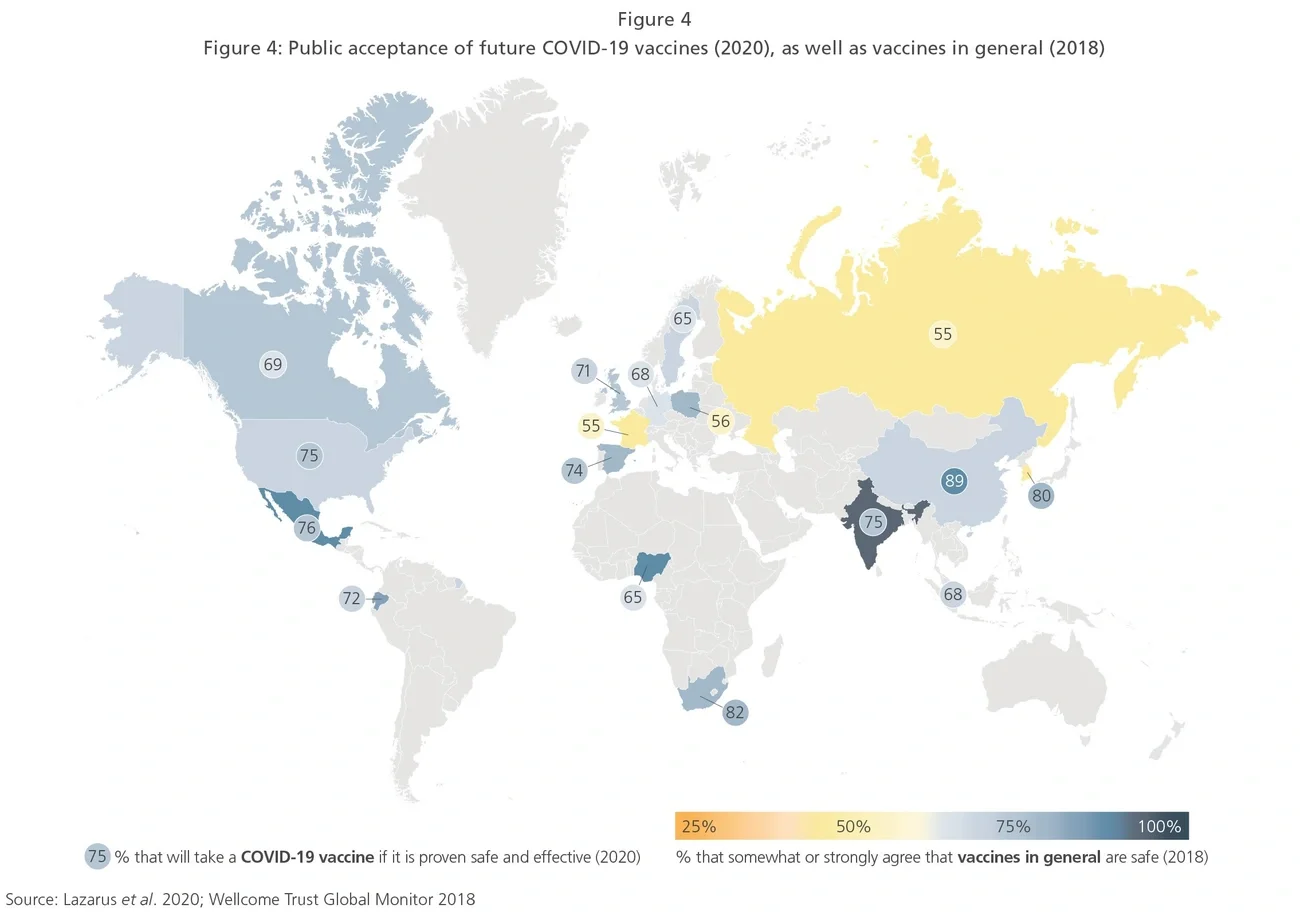
Countries are about to embark on one of the largest and most logistically challenging vaccine roll-outs ever witnessed and, as they do so, one of the biggest lessons may yet be to come: how to overcome the increasing problem of vaccine “hesitancy.” A study published in The Lancet in October 2020 revealed the scale of this challenge in countries such as Russia and France (see Exhibit 4). However, optimistically, in many countries the degree of confidence in a COVID- 19 vaccine was often higher than that generally seen for vaccines overall. We can hope that a successful COVID-19 vaccine roll-out could serve as a reminder of the power and importance of vaccines more generally.