Obesity continues to affect a disproportionately large number of people. With the prevalence of glucagon-like peptide-1 (GLP-1) drugs, more individuals are recognizing obesity for what it is: a chronic disease, rather than a condition caused by a lack of willpower. As GLP-1 uptake continues, weight management solutions, including structured weight management programs (SWMPs) like WeightWatchers (WW) and Noom, may still have a place in the shifting paradigm of obesity treatment.
After all, although obesity medications initially disrupted SWMPs, growing evidence shows that patients should not neglect diet and exercise to achieve optimal, long-term results. SWMPs may also help address gaps in care that currently exist with overburdened primary care providers.
This Executive Insights discusses several trends in the SWMP market:
- Riding the GLP-1 trend away from “diet culture”
- The virtual way or the highway
- Partnership-fueled growth
At this pivotal time, SWMPs must evolve strategically from their traditional model, which some perceive as promoting diet culture, to stay in tune with changing consumer preferences. SWMPs need to demonstrate their complementarity to GLP-1s in earnest and navigate the weight management space aptly.
Obesity as a chronic condition
In 2013, the American Medical Association recognized obesity as a complex, chronic disease requiring medical attention. Although the public has been slow to accept obesity as a medical condition, often seeing it as a behavioral issue, this sentiment has been shifting with the increasing prevalence of GLP-1s. Unlike historically unsuccessful and damaging drugs such as rainbow diet pills and fen-phen, GLP-1s show considerable promise, underscoring that obesity can be treated pharmacologically and is, in fact, an illness.
These new drugs are reshaping not only how obesity is treated but also how it is perceived — as a persistent medical condition stemming from biological factors, not merely a matter of self-discipline or resolve.
A body mass index (BMI) of 30 or more characterizes obesity in adults, whereas a BMI over 40 characterizes severe obesity. Obesity is widespread in the U.S., affecting 42.4% of adults (over 140 million Americans), with 9.2% classified as severely obese (over 30 million Americans). According to national surveys conducted since the early 1960s, obesity rates in the U.S. have tripled over the past 60 years and are expected to continue to rise. A study led by Harvard T.H. Chan School of Public Health predicts that by 2030, around 50% of the U.S. adult population will have obesity, with about a quarter experiencing severe obesity.
The future of weight management and SWMPs
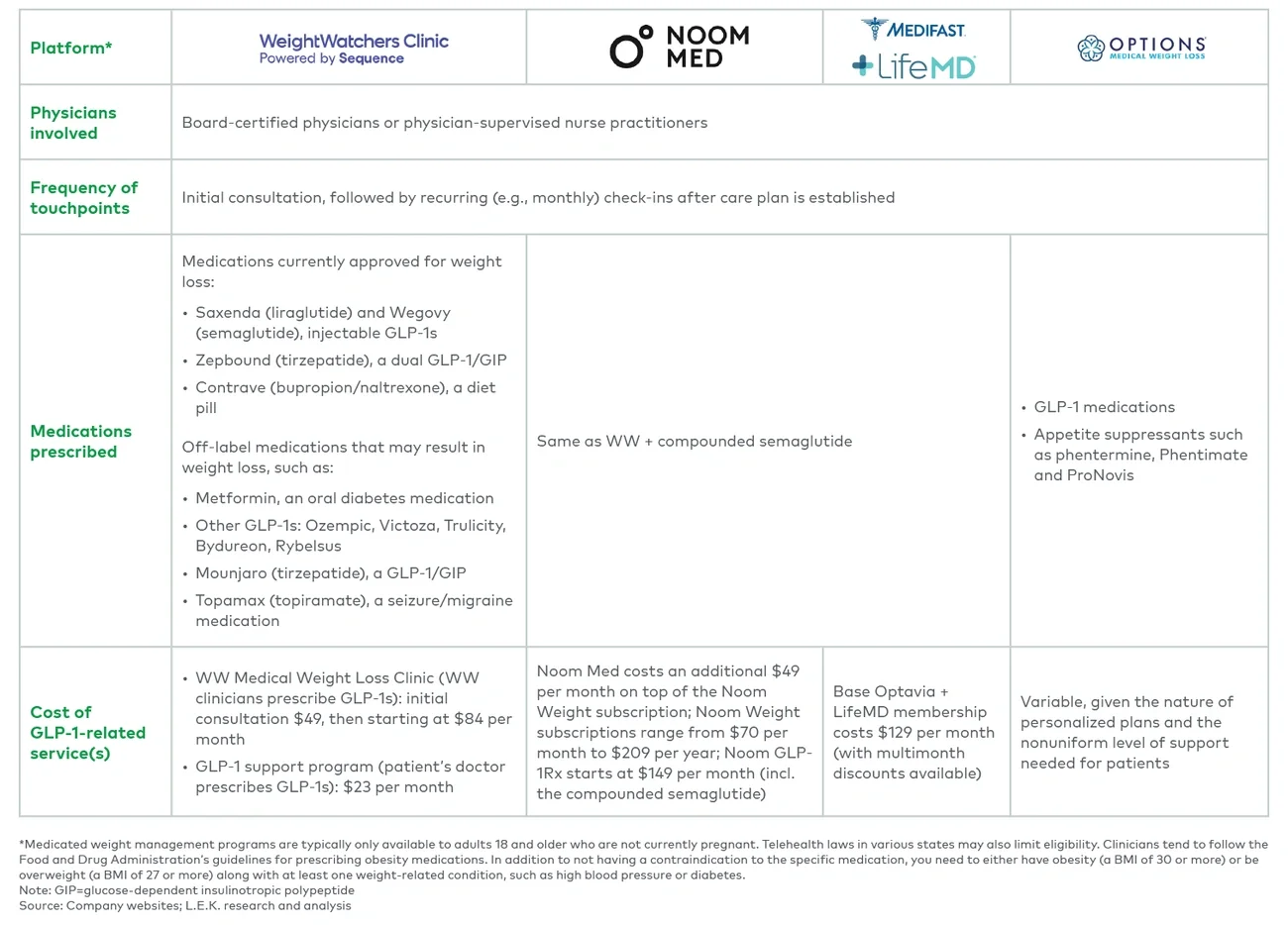
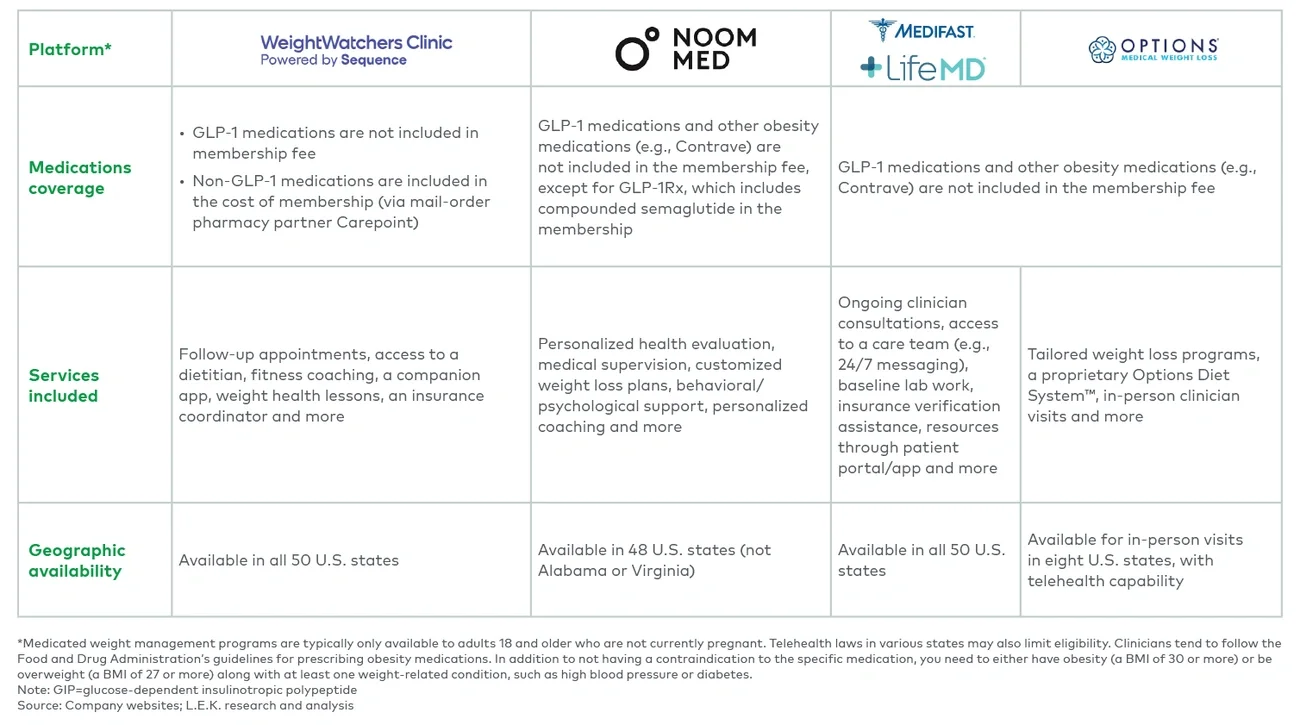
As obesity continues to prevail, even as GLP-1s grow in popularity, individuals will continue to seek various weight management and obesity treatment options, ranging from diet food and drinks to health clubs and medical interventions. Weight management products and services may be particularly attractive to patients using GLP-1s, as evidence increasingly shows that diet and exercise should not be neglected to achieve optimal, long-term results. Specifically, SWMPs like WW and Noom (see Figure 1), initially disrupted by GLP-1s, now emphasize their complementarity to these obesity drugs.
SWMPs are traditionally seen as “integrated solutions,” combining both products and services within a well-designed program. They typically serve individuals who have not seen desired results from other do-it-yourself approaches to weight loss, historically focusing on dieting. Many SWMPs have publicly acknowledged obesity as a disease that requires personalized treatment, have introduced GLP-1-related offerings, and have highlighted that they may be able to help fill care gaps in treating obesity with medications. After all, numerous primary care doctors, who often prescribe GLP-1s, may not be trained in obesity medicine or have the time to educate patients comprehensively.